Technological breakthroughs in modern healthcare have paved the path for novel techniques that not only improve diagnostic precision but also provide effective therapeutic approaches. Endoscopic Retrograde Cholangiopancreatography, or ERCP, is one such procedure that sits at the intersection of endoscopy, radiology, and gastroenterology. This complicated medical procedure has transformed the diagnosis and treatment of bile duct, liver, gallbladder, and pancreas problems.
In this comprehensive guide, we embark on a journey to decode the intricacies of ERCP, shedding light on its purpose, procedural nuances, potential benefits, associated risks, and the crucial phase of post-procedure recovery. As we delve into the depths of ERCP, we aim to provide a clear and accessible understanding of this remarkable procedure. Whether you’re a patient preparing for an upcoming ERCP or simply intrigued by the marvels of medical science, this guide aims to unravel the complexities and demystify ERCP’s role in modern healthcare.
Understanding ERCP: Purpose and Significance
ERCP is a critical diagnostic and therapeutic treatment in the field of gastroenterology. Its goal is to meticulously examine and manipulate the biliary and pancreatic channels, allowing clinicians to identify and treat a variety of gastric issues affecting essential systems. ERCP is critical in identifying blockages, gallstones, tumors, and other abnormalities inside the bile and pancreatic ducts, providing insights that would be difficult to obtain with other imaging modalities.
Furthermore, the significance of the ERCP procedure extends to its therapeutic potential, allowing for procedures like gallstone removal, stent implantation to ease blockages, and even biopsy collection. ERCP has become a vital technique in managing a variety of hepatopancreatobiliary illnesses, improving patient outcomes and quality of life by permitting both diagnostic clarity and less invasive therapies.
Common Conditions Diagnosed With ERCP
ERCP (Endoscopic Retrograde Cholangiopancreatography) is a flexible treatment used to identify and treat biliary and pancreatic problems. ERCP is commonly used to diagnose and treat the following conditions:

1. Gallstones
ERCP is usually performed to remove gallstones that have migrated from the gallbladder into the bile ducts, creating obstruction and potentially leading to discomfort, jaundice, or infection.
2. Biliary Obstructions
This is a medical condition characterized by the blockage of the bile ducts that carry bile from the liver to the small intestine. ERCP stands as a cornerstone in the assessment and management of biliary obstructions, providing both diagnostic insights and therapeutic solutions.
3. Biliary Pancreatic Duct Disorders
ERCP can detect bile ducts and pancreatic duct abnormalities such as dilatation, strictures, and irregularities. These findings may help to guide future treatment.
4. Biliary and Pancreatic Tumors
ERCP can help with the visibility and biopsy of tumors in the bile ducts or pancreas, which can help with the diagnosis and stage of these cancers.
5. Cholangitis
ERCP can be performed to treat acute cholangitis, a bile duct infection caused by a bacterial blockage. The technique can assist in removing the blockage and alleviating the illness.
The ERCP Procedure: Step by Step
ERCP is a medical treatment used to diagnose and treat bile and pancreatic duct disorders. An endoscope which is a flexible tube with a camera and light at its tip that is passed into the mouth, esophagus, stomach, and into the small intestine, is used. The ERCP process is described in detail below:
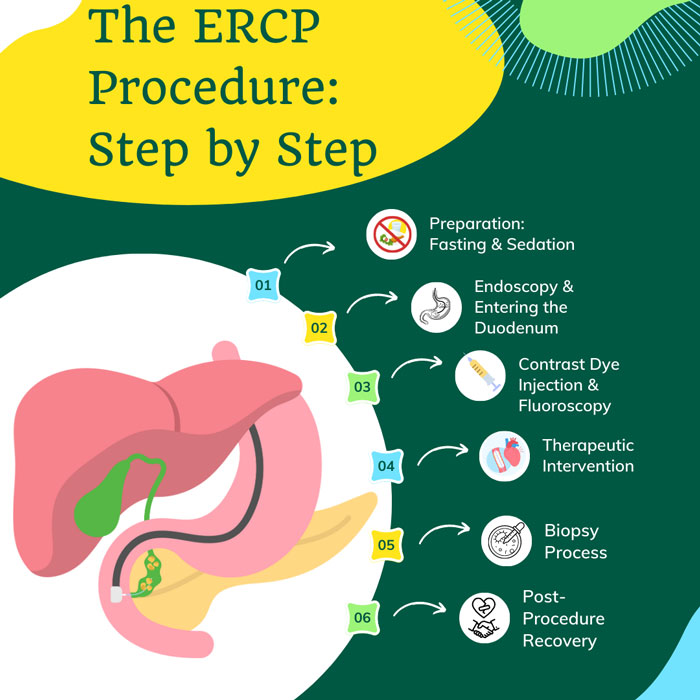
1. Preparation: Fasting Sedation
Fasting and sedation are two vital components of ERCP preparation. Fasting is required to ensure that the bile and pancreatic ducts can be seen clearly during the operation. Patients usually needed to fast for a certain amount of time, sometimes overnight. It is because the presence of food particles in the digestive tract can impede vision or interfere with the process. Sedation, on the other hand, tries to give the patient comfort and relief from anxiety. An anesthesiologist administers it to create a regulated state of relaxation or sleep, allowing the endoscopist to execute the surgery more effectively while lowering patient discomfort.
2. Endoscopy Entering the Duodenum
The next step in an ERCP surgery is to carefully move an endoscope into the duodenum. In order to track the upper gastrointestinal tract, performing Endoscopic Ultrasound is a crucial procedure. Following adequate patient preparation and anesthesia, the endoscopist inserts the endoscope cautiously via the patient’s mouth, traveling through the esophagus and stomach before reaching the duodenum. The endoscopist must negotiate anatomical curves and guarantee a smooth passage to the target area during this stage of the process, which demands precision and patience.
3. Contrast Dye Injection Fluoroscopy
Following an ERCP procedure’s successful entrance into the duodenum, contrast dye injection, and fluoroscopy are the next steps. This is essential for understanding the complex system of bile and pancreatic ducts. A tiny catheter is delicately inserted into the appropriate duct opening through the working channel of the endoscope once it has been positioned close to the duodenum. The duct is then carefully filled with a contrast dye, which is then allowed to pass through the ductal system. Fluoroscopy, a real-time X-ray imaging method, is also used to record dynamic pictures of the dye’s motion. By combining these two methods, a thorough map of the ductal routes is produced, showing any potential anomalies, blockages, or irregularities.
4. Therapeutic Interventions
After contrast dye injection and fluoroscopy, therapeutic interventions take center stage in the arena of an ERCP process. Stent implantation and dilatation, are critical in the treatment of a variety of biliary and pancreatic illnesses. Stent placement is carefully inserting a tiny tube-like device into restricted or clogged ducts, restoring adequate bile or pancreatic flow. This method is especially useful in cases of ductal strictures or blockages caused by diseases such as gallstones or tumors. The ERCP surgery provides patients with effective relief from obstructive difficulties and contributes to improving their overall quality of life by utilizing therapeutic procedures such as stent insertion and dilatation.
5. Biopsy Process If a Necessary
Biopsy is determined necessary to further examine a potential anomaly during an ERCP operation, the technique is carried out with accuracy. Once the endoscope is in the duodenum and the target location is identified under fluoroscopic guidance, the endoscopist uses specialized equipment to perform the biopsy. To reduce discomfort, a local anesthetic can be used. The endoscopist gently collects a small tissue sample from a suspicious location, such as a lesion, stricture, or mass, using biopsy forceps passed via the working channel of the endoscope. This sample is then recovered and kept for laboratory analysis.
6. Post-Procedure Recovery
After the ERCP, patients are carefully transferred to a separate recovery area. In this case, constant monitoring by healthcare personnel ensures a smooth transition from sedation to wakefulness. To assess the patient’s stability, vital signs such as heart rate, blood pressure, and oxygen levels are continuously monitored. Patients eventually awaken from the procedure-induced lethargy as the sedative effects wear off. If pain management measures are required, they are implemented. To avoid aspiration, patients are usually advised to refrain from eating or drinking while the gag reflex returns.
ERCP’s Diagnostic and Therapeutic Significance
In the realm of gastroenterology, ERCP has significant diagnostic and therapeutic implications. As a diagnostic technique, ERCP enables clinicians to clearly examine and assess the bile and pancreatic ducts, assisting in the diagnosis of problems such as gallstones, strictures, tumors, and infections. Its distinct ability to provide a direct view of these complicated structures frequently removes the need for more invasive exploratory procedures. Furthermore, the therapeutic promise of ERCP is compelling. It allows for specific treatments like stent implantation, dilatation, and biopsy within the same process, reducing the need for further invasive procedures.
As a result, ERCP is a helpful procedure for removing blockages, improving correct fluid flow, and treating a variety of biliary and pancreatic illnesses. ERCP’s dual function in diagnosing and treating complex illnesses has transformed patient care, providing precise diagnoses and effective therapies that can greatly enhance patient outcomes and quality of life.
Potential Risks Complications Associated With ERCP
Healthcare professionals use ERCP to diagnose and treat biliary, gallbladder, and pancreatic disorders. Although ERCP is safe and effective, there are still some risks and complications. It’s crucial to remember that the risk of these consequences varies depending on the patient’s overall health, the specifics of the surgery, and the experience of the medical team doing the ERCP. The following are some possible risks and complications:
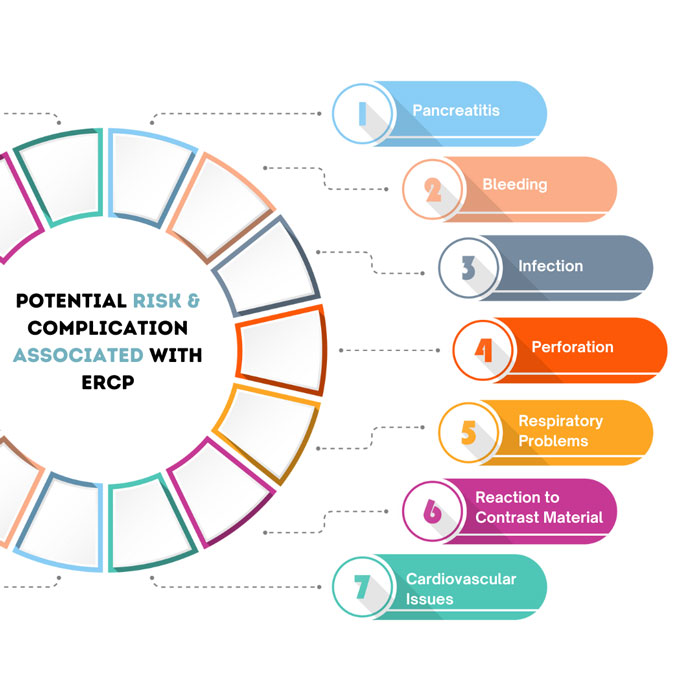
1. Pancreatitis
This is one of the most common and dangerous complications of ERCP. It is characterized by pancreatic inflammation which is a sign that you have gastric problems that can range from mild to severe. Severe pancreatitis can result in hospitalization and potentially fatal complications.
2. Bleeding
ERCP involves inserting devices into the digestive tract, which can cause blood vessel damage and bleeding. Mild bleeding may resolve on its own, but excessive bleeding may necessitate additional medical attention.
3. Infection
ERCP involves the use of endoscopic instruments and can introduce bacteria into the digestive tract, potentially leading to infections.
4. Perforation
There is little danger of perforating (tearing a hole in) the digestive tract wall during ERCP. This can result in infection, peritonitis (abdominal lining inflammation), and other problems.
5. Reaction to Contrast Material
ERCP frequently includes the injection of a contrast dye to improve visualization of the bile ducts and pancreatic ducts. Some people may be allergic to the contrast material, which can range from mild to severe.
6. Respiratory Problems
Regular sedation or anesthesia during ERCP could lead to respiratory problems, such as shallow breathing or even respiratory distress.
7. Cardiovascular Issues
The use of Sedation and anesthesia during ERCP can have a negative impact on the cardiovascular system, altering blood pressure and heart rate.
Before having ERCP, patients should have a full discussion with their doctor about any possible dangers and advantages. To decide whether ERCP is necessary and to reduce the dangers involved with the treatment, healthcare professionals will evaluate each patient’s unique medical history, present health status, and specific problems.
Preparing for ERCP: Patient’s Perspective
Preparing for an ERCP surgery is a combination of anticipation and essential preparations from the patient’s standpoint. Patients should anticipate receiving full instructions from their healthcare provider before surgery. Fasting instructions are typically provided to ensure a clear digestive tract, which aids in the effectiveness and safety of the treatment. It is crucial to follow these pre-procedure recommendations because it allows for the finest possible view of the bile and pancreatic ducts during the ERCP. Another critical aspect of preparation is to address any concerns about sedation and anesthesia.
Patients can express their concerns to their healthcare provider, gaining a better knowledge of the medication use and the level of comfort expected during the treatment. This communication reduces worry and promotes a sense of preparedness. Having a thorough understanding of the procedures leading up to the ERCP enables patients to actively participate in their own healthcare experience, creating a more seamless and knowledgeable interaction.
The ERCP Experience: Patient Recovery and Follow-Up
The ERCP experience includes not only the procedure but also the critical stages of patient recovery and follow-up care. Following surgery, healthcare professionals carefully observe patients as they gradually regain consciousness during a post-procedure recovery phase. The duration of recovery varies, with some patients being able to go home the same day and others requiring overnight observation. While soreness, bloating, or moderate side effects may occur, medical professionals provide assistance on how to manage these difficulties to facilitate a more comfortable recovery.
This recuperation phase is critical for patients to rest and gradually resume their normal activities. The journey, however, does not finish here. It is impossible to overestimate the importance of follow-up appointments. Healthcare personnel analyze the ERCP results, explain any biopsy findings, and assess the patient’s recovery status.
The Bottom Line
Navigating the world of medical procedures can be less intimidating when armed with knowledge. This comprehensive guide has shed light on the intricate yet vital procedure of ERCP, demystifying its purpose, process, and potential outcomes. Whether used for diagnosis or treatment, ERCP stands as a valuable tool in managing conditions related to the bile and pancreatic ducts. Remember, effective communication with your healthcare provider is key; don’t hesitate to ask questions and discuss any concerns you may have. For the best health advice tailored to your individual needs, you can consult Dr. Preetha Thomas, who can provide expert guidance and support on your medical journey. With the right information and medical care, you can approach ERCP and other procedures with confidence.