You don’t drink alcohol—or maybe you have an occasional glass of wine. You’re not an alcoholic, so when your doctor mentions “fatty liver disease” after routine blood work, you’re confused and maybe a little offended. How can you have liver disease when you barely drink?
Welcome to one of the most misunderstood health conditions of our time: non-alcoholic fatty liver disease (NAFLD). It’s now the most common liver condition worldwide, affecting an estimated 25-30% of adults in Western countries. And it has nothing to do with alcohol consumption.
What Is Fatty Liver Disease?
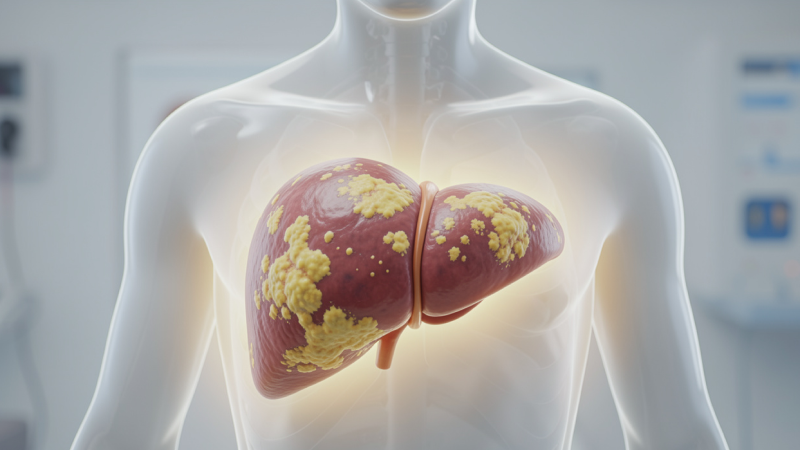
Your liver is supposed to process fat, not store it. But when your liver accumulates excess fat—specifically, when more than 5-10% of your liver’s weight is fat—you have fatty liver disease. Think of it like your liver becoming a storage unit instead of a processing plant.
Non-alcoholic fatty liver disease occurs when this fat accumulation happens in people who drink little to no alcohol. For many people, fatty liver causes no symptoms and may never progress beyond fat storage. But for others, it can advance to inflammation (non-alcoholic steatohepatitis or NASH), scarring (fibrosis), cirrhosis, and even liver failure or liver cancer.
The scary part? Most people have no idea they have it until it’s discovered incidentally during imaging for something else, or until liver function tests come back abnormal.
The Real Culprits Behind Fatty Liver
If alcohol isn’t the cause, what is? The answer lies in modern lifestyle factors that have created a perfect storm for liver disease.
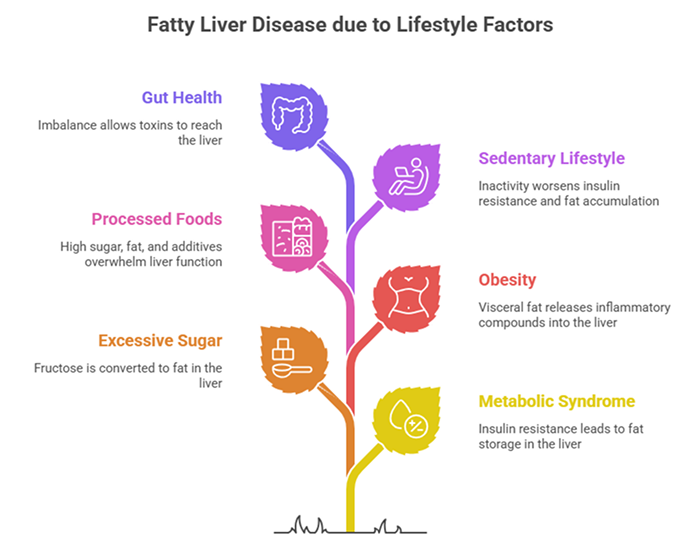
Metabolic Syndrome and Insulin Resistance
The biggest driver of fatty liver is metabolic syndrome—a cluster of conditions including high blood pressure, high blood sugar, excess abdominal fat, and abnormal cholesterol levels. These conditions are all linked by insulin resistance, where your cells don’t respond properly to insulin.
When you’re insulin resistant, your liver converts excess glucose into fat and stores it. Over time, this fat accumulation overwhelms your liver’s ability to process and export it. Your liver essentially becomes a fat storage depot.
You don’t need to be diabetic to have insulin resistance. Many people with normal blood sugar readings already have significant insulin resistance developing in the background. By the time blood sugar becomes elevated, insulin resistance has often been present for years—and so has fatty liver.
The Sugar Connection
Excessive sugar consumption, particularly fructose, is devastating to your liver. Unlike glucose, which can be used by all your body’s cells, fructose is processed almost exclusively in your liver. When you consume large amounts of fructose—from soda, fruit juice, processed foods with high-fructose corn syrup, or even excessive fruit consumption—your liver converts it directly into fat.
This isn’t about natural sugars in whole fruits eaten in reasonable amounts. It’s about the massive doses of concentrated fructose in modern diets. A single can of soda can contain 40+ grams of sugar, much of it fructose. Your liver simply wasn’t designed to handle this metabolic load.
Research shows that high sugar consumption directly contributes to fatty liver development, independent of total calorie intake or weight gain.
Obesity and Excess Abdominal Fat
Carrying excess weight, particularly around your midsection, significantly increases fatty liver risk. Visceral fat (the deep abdominal fat surrounding your organs) is metabolically active, releasing inflammatory compounds and free fatty acids directly into your bloodstream. Your liver must process these fats, and over time, it becomes overwhelmed.
Even people who aren’t technically obese but carry excess belly fat are at risk. You can have a “normal” BMI but still have dangerous amounts of visceral fat—a condition sometimes called “skinny fat” or metabolically obese normal weight.
The Ultra-Processed Food Diet
Modern diets dominated by processed foods contribute to fatty liver in multiple ways. These foods are typically high in refined carbohydrates, added sugars, unhealthy fats, and sodium while being low in fiber and nutrients. This combination promotes insulin resistance, inflammation, and fat storage in the liver.
Additionally, many processed foods contain additives, preservatives, and other compounds that your liver must process and detoxify. The constant burden of processing these substances while simultaneously dealing with excess sugar and fat overwhelms liver function.
Sedentary Lifestyle
Physical inactivity is a major risk factor for fatty liver. Exercise helps your body use glucose efficiently, improves insulin sensitivity, reduces inflammation, and helps burn the fat stored in your liver. When you’re sedentary, glucose isn’t efficiently used by muscles, insulin resistance worsens, and fat accumulates in your liver.
The modern lifestyle of sitting for 8-10 hours daily—at work, during commutes, at home watching TV—creates the perfect conditions for metabolic dysfunction and fatty liver development.
Gut Health and Microbiome Imbalance
Emerging research shows strong connections between gut health and fatty liver. Your gut microbiome—the trillions of bacteria in your intestines—influences metabolism, inflammation, and fat storage. An imbalanced microbiome (dysbiosis) can increase intestinal permeability (“leaky gut”), allowing bacterial toxins to enter your bloodstream and reach your liver, triggering inflammation and fat accumulation.
Factors that disrupt gut health—antibiotics, poor diet, chronic stress, lack of fiber—all indirectly contribute to fatty liver development.
Why You Might Not Have Symptoms
Here’s the frustrating part: fatty liver rarely causes obvious symptoms in its early stages. Your liver doesn’t have pain receptors, so it can be significantly damaged before you feel anything. When symptoms do appear, they’re often vague:
- Persistent fatigue
- Vague discomfort in the upper right abdomen
- Unexplained weight changes
- Difficulty losing weight despite diet efforts
By the time obvious symptoms appear—yellowing skin (jaundice), abdominal swelling, confusion—the disease has often progressed to advanced stages like cirrhosis.
This is why routine blood work and screenings are crucial. Elevated liver enzymes (ALT and AST) can be early warning signs, though some people with fatty liver have normal enzyme levels.
Who’s at Highest Risk?
Certain factors significantly increase your risk of developing fatty liver:
- Type 2 diabetes or prediabetes
- Obesity, especially with abdominal fat
- High triglycerides or low HDL cholesterol
- Metabolic syndrome
- Polycystic ovary syndrome (PCOS)
- Sleep apnea
- Hypothyroidism
- Age over 50
- Family history of fatty liver or diabetes
However, younger people are increasingly developing fatty liver, even teenagers and children, primarily due to rising obesity rates and poor dietary habits.
What You Can Do About It
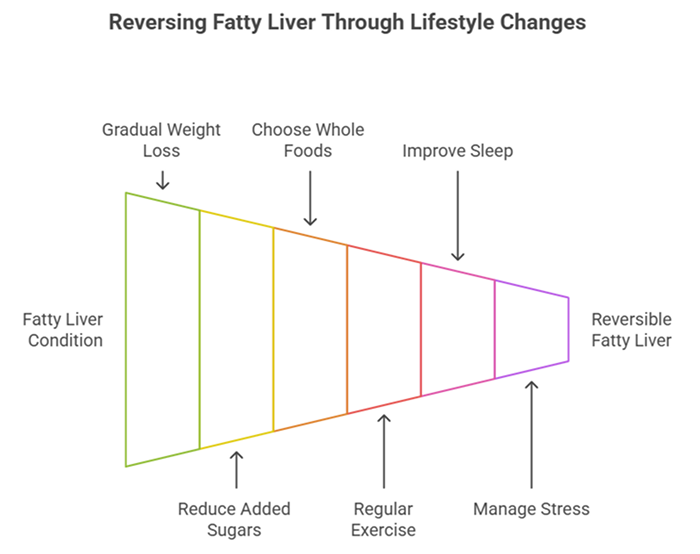
The good news is that fatty liver is largely reversible, especially in its early stages. Unlike many liver conditions, you have significant control over fatty liver through lifestyle changes.
Lose Weight Gradually
Even modest weight loss—5-10% of your body weight—can significantly reduce liver fat. Rapid weight loss can actually worsen liver inflammation, so aim for slow, steady weight loss of 1-2 pounds per week.
Focus on sustainable dietary changes rather than extreme diets. The goal is long-term lifestyle modification, not temporary restriction.
Cut Out Added Sugars
This is perhaps the most important dietary change. Eliminate or drastically reduce:
- Sugary beverages (soda, sweetened coffee drinks, fruit juices)
- Candy and desserts
- Processed foods with added sugars
- Foods with high-fructose corn syrup
Read labels carefully. Sugar hides under many names in processed foods.
Choose Whole, Unprocessed Foods
Build your diet around:
- Vegetables (especially leafy greens)
- Whole fruits (in moderation)
- Lean proteins (fish, poultry, legumes)
- Whole grains
- Healthy fats (olive oil, avocados, nuts)
- Fiber-rich foods
These foods support liver health, improve insulin sensitivity, and provide nutrients needed for liver function and repair.
Exercise Regularly
Both aerobic exercise and resistance training help reduce liver fat. Aim for at least 150 minutes of moderate-intensity exercise weekly. Exercise improves insulin sensitivity, helps burn liver fat, and supports overall metabolic health.
Even without weight loss, exercise can reduce liver fat and improve liver function. Movement is medicine for fatty liver.
Improve Sleep Quality
Poor sleep and sleep apnea are associated with fatty liver. Prioritize 7-9 hours of quality sleep nightly. If you snore heavily or feel tired despite adequate sleep time, get evaluated for sleep apnea.
Manage Stress
Chronic stress affects metabolism, promotes inflammation, and can worsen insulin resistance. Implement stress-reduction practices like meditation, yoga, or regular relaxation time.
Stay Properly Hydrated
Adequate hydration supports liver function and helps your body process and eliminate toxins. Drink water throughout the day.
When to See a Gastroenterologist
If you have risk factors for fatty liver, elevated liver enzymes on blood work, or any concerning symptoms, professional evaluation is important. A gastroenterologist can:
- Perform imaging studies to assess liver fat and damage
- Determine if you have simple fatty liver or more advanced disease
- Rule out other liver conditions
- Provide personalized treatment recommendations
- Monitor disease progression
Early intervention makes a tremendous difference. Fatty liver caught early is highly reversible. Advanced disease with significant scarring is much harder to reverse.
The Bottom Line
Fatty liver disease isn’t just about alcohol. For millions of people, it’s about the cumulative effects of modern lifestyle—too much sugar, too many processed foods, too little movement, too much stress, and too little sleep. Your liver is paying the price for these factors, silently accumulating fat and inflammation.
The condition is serious—it can progress to cirrhosis and liver failure. But it’s also largely preventable and reversible through lifestyle changes. You have more control over your liver health than you might think. Start with small, sustainable changes. Your liver has remarkable regenerative capacity when given the chance to heal.
If you’re experiencing warning signs of liver problems or have risk factors for liver disease, Dr. Preetha Thomas, specialist gastroenterologist with expertise in hepatology in Pretoria, provides comprehensive liver evaluation and personalized treatment plans.
Contact us today to schedule your consultation.