You wake up with a bitter, metallic taste coating your mouth. Or maybe it hits you randomly throughout the day—that unpleasant, acrid flavor that won’t go away no matter how much you brush your teeth or rinse with mouthwash. You pop a mint, chew gum, drink water, but within minutes, that awful taste creeps back.
It’s more than just annoying. It affects how you enjoy food, makes you self-conscious about your breath, and leaves you wondering what’s wrong. You’ve probably googled it (that’s likely how you found this article), and the internet has probably terrified you with worst-case scenarios.
Here’s what I want you to know: while a persistent bitter taste can indicate health issues, it’s rarely something catastrophic. More often, it’s your body’s way of telling you something’s off with your digestive system. Let me walk you through the most common digestive causes and what you can actually do about them.
The Acid Reflux Connection: The Most Common Culprit
Let’s start with the big one. If you have a bitter or sour taste in your mouth, especially in the morning or after meals, acid reflux is probably to blame. This is by far the most common digestive cause of bitter taste.
Here’s what’s happening: your stomach produces hydrochloric acid to digest food. Normally, a muscular valve called the lower esophageal sphincter keeps stomach contents where they belong. But when this valve weakens or relaxes inappropriately, stomach acid flows backward into your esophagus and sometimes all the way up to your throat and mouth.
That acid tastes awful—bitter, sour, metallic. Even if you don’t feel the classic “heartburn” burning sensation in your chest, you might still have what’s called “silent reflux” where the main symptom is this persistent bad taste, along with throat clearing, hoarseness, or a chronic cough.
Why does reflux cause bitter taste specifically in the morning? Because when you lie down to sleep, gravity stops helping keep acid down. If you ate dinner late, or had trigger foods like coffee, alcohol, chocolate, or fatty meals, acid is more likely to creep up overnight. You wake up with that disgusting taste coating your mouth.
The reflux-bitter taste connection often comes with other clues: you might notice the taste worsens after eating certain foods, you feel it more when you bend over or lie down, or you experience occasional heartburn or chest discomfort. If any of this sounds familiar, acid reflux is probably your answer.
Bile Reflux: The Lesser-Known Troublemaker
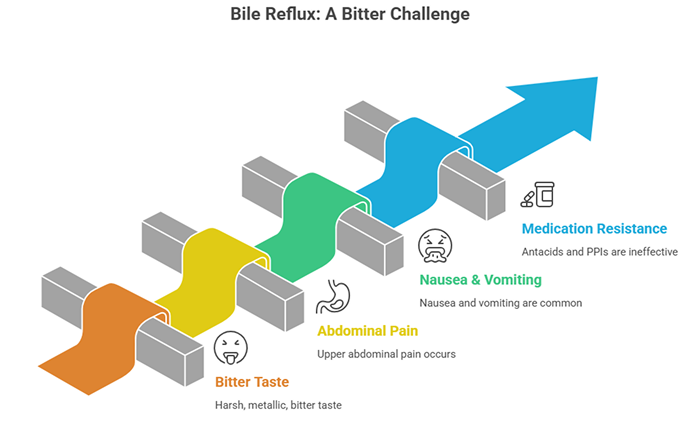
Here’s something most people don’t know about: bile reflux. While similar to acid reflux, this involves bile—a digestive fluid produced by your liver—flowing backward from your small intestine into your stomach and esophagus.
Bile tastes intensely bitter. It’s designed to break down fats in your small intestine, not to be anywhere near your mouth. When it refluxes up, it creates a particularly harsh, bitter metallic taste that’s often described as worse than regular acid reflux.
Bile reflux can happen along with acid reflux or on its own. It’s more common in people who’ve had gallbladder surgery, stomach surgery, or peptic ulcers. The bitter taste from bile reflux is often accompanied by upper abdominal pain, nausea, and sometimes vomiting of greenish-yellow fluid.
Unlike regular acid reflux which improves with antacids, bile reflux doesn’t respond as well to standard reflux medications. That’s an important clue—if you’re taking antacids or PPIs (proton pump inhibitors) and the bitter taste persists, bile reflux might be the actual problem.
Gastroparesis: When Your Stomach Forgets How to Empty
Gastroparesis is a condition where your stomach empties too slowly. Food sits there, fermenting and creating gas, and that partially digested content can reflux back up, creating a bitter or sour taste.
People with diabetes are particularly prone to gastroparesis because high blood sugar can damage the vagus nerve that controls stomach emptying. But you can develop it from other causes too—viral infections, certain medications, or sometimes for unknown reasons.
The bitter taste from gastroparesis usually comes with other symptoms: feeling full after eating very little, bloating, nausea (especially after meals), and sometimes vomiting hours after eating. If this sounds like you, especially if you’re diabetic, gastroparesis could be contributing to that bitter taste.
Small Intestinal Bacterial Overgrowth (SIBO): The Bacterial Imbalance
Your small intestine is supposed to have relatively few bacteria compared to your large intestine. But sometimes bacteria migrate upward and overgrow where they shouldn’t be. This is SIBO—small intestinal bacterial overgrowth.
When you have SIBO, these misplaced bacteria ferment the food you eat, producing gases and various compounds. Some of these compounds can reflux upward, creating bitter or metallic tastes. The taste might be accompanied by significant bloating (especially after eating carbohydrates), gas, diarrhea or constipation, and general digestive discomfort.
SIBO is often overlooked as a cause of bitter taste, but it’s more common than most people realize. It frequently develops after food poisoning, following antibiotic use, or in people with slow gut motility or structural abnormalities in the digestive tract.
Liver and Gallbladder Issues: The Bile Connection
Your liver produces bile, and your gallbladder stores and concentrates it. When something’s wrong with either organ, bile flow can be disrupted, potentially causing bitter taste.
Gallstones, for instance, can block bile ducts, causing bile to back up. This can create a bitter taste along with pain in the upper right abdomen, especially after eating fatty meals. The pain might radiate to your back or shoulder blade.
Liver problems—whether from fatty liver disease, hepatitis, cirrhosis, or other conditions—can affect bile production and create taste changes. If the bitter taste is accompanied by yellowing of your skin or eyes (jaundice), dark urine, pale stools, or persistent fatigue, liver issues should definitely be investigated.
Medications and Your Digestive System
Hundreds of medications can cause bitter or metallic tastes, and many work through digestive mechanisms. Some common culprits include:
Antibiotics (particularly metronidazole and clarithromycin) are notorious for creating metallic tastes. They alter your gut bacteria and can irritate your digestive tract. Blood pressure medications, especially ACE inhibitors and calcium channel blockers, frequently cause taste changes. Diabetes medications like metformin can create metallic tastes and also slow stomach emptying. Antidepressants, particularly SSRIs, affect taste perception and can slow digestion.
The timing is usually a giveaway—if the bitter taste started shortly after beginning a new medication, that’s probably your answer. Don’t stop taking prescribed medications without talking to your doctor, but definitely mention the taste issue. There might be alternatives.
Poor Oral Hygiene and the Gut Connection
I know this sounds obvious, but hear me out. Poor oral hygiene doesn’t just affect your mouth—it affects your entire digestive system. The bacteria in your mouth are the first stop in your digestive tract. When you have gum disease, tooth decay, or chronic bad oral hygiene, harmful bacteria proliferate in your mouth.
These bacteria produce sulfur compounds and other substances that taste bitter and foul. They can also travel down to your stomach and alter your gut microbiome. Additionally, oral infections and inflammation can change your taste perception.
But here’s the digestive connection: conditions like acid reflux and bile reflux can actually cause or worsen oral health problems. The acid and bile damage tooth enamel and irritate gum tissue. So sometimes oral issues and digestive issues create a vicious cycle—each making the other worse.
Smoking and Digestive Function
If you smoke, that might be contributing to your bitter taste in multiple ways. Obviously, smoking directly affects how things taste and creates that characteristic smoker’s breath. But beyond the direct effects, smoking significantly impacts digestive health.
Nicotine relaxes the lower esophageal sphincter, making acid reflux more likely. Smoking reduces saliva production—and saliva is your mouth’s natural cleaning and neutralizing system. Less saliva means tastes (including bitter ones) linger longer. Smoking also increases stomach acid production while simultaneously irritating the stomach lining, creating a setup for reflux and that bitter taste.
Dehydration: The Simple Factor That’s Often Overlooked
When you’re dehydrated, you produce less saliva. Saliva is crucial for washing away food particles, neutralizing acids, and maintaining normal taste perception. Without adequate saliva, everything tastes off—often bitter or metallic.
Dehydration also thickens mucus in your throat and mouth, which can trap bacteria and create bitter tastes. Additionally, many people don’t realize that adequate water intake is essential for proper digestive function. When you’re dehydrated, digestion slows, which can worsen reflux and other digestive issues that contribute to bitter taste.
The fix is simple: drink more water throughout the day. Your urine should be pale yellow. If it’s darker, you’re not drinking enough.
Stress and the Gut-Brain-Taste Connection
Chronic stress affects your digestive system in profound ways, and taste perception is part of that. When you’re stressed, your body produces more stomach acid, which increases reflux risk. Stress also slows digestion, allowing food to sit in your stomach longer and potentially reflux upward.
Beyond the physical effects, stress directly alters taste perception. Many people report that foods taste different—often more bitter or metallic—during periods of high stress or anxiety. The gut-brain connection is powerful, and taste is very much part of this communication system.
If your bitter taste worsens during stressful periods or comes with other stress-related digestive symptoms like stomachaches or diarrhea, stress management isn’t optional—it’s part of your treatment.
What You Can Actually Do About It
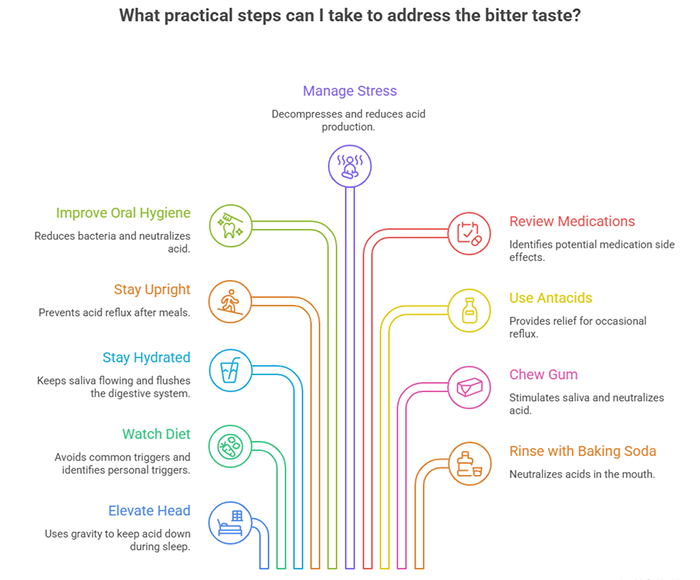
Okay, so you recognize yourself in one or more of these causes. What now? Here are practical steps that actually help:
Elevate your head while sleeping. If reflux is your issue (and it probably is), raise the head of your bed 6-8 inches using bed risers or a wedge pillow. This uses gravity to keep acid down. Just piling up regular pillows doesn’t work—you need your entire torso elevated.
Watch when and what you eat. Stop eating at least three hours before bed. Avoid common reflux triggers: coffee, alcohol, chocolate, spicy foods, fatty foods, citrus, and tomatoes. Pay attention to what makes YOUR bitter taste worse—everyone’s triggers are slightly different.
Stay hydrated throughout the day. Sip water regularly. This keeps saliva flowing and helps flush your digestive system.
Don’t lie down right after eating. Stay upright for at least two to three hours after meals. Take a walk, do dishes, engage in light activity—just don’t lie on the couch or go straight to bed.
Improve your oral hygiene. Brush twice daily, floss, use mouthwash, and see your dentist regularly. If you have the bitter taste, brush your tongue too—that’s where bacteria accumulate.
Manage your stress. I know, easier said than done. But find something that works for you—exercise, meditation, therapy, hobbies, whatever helps you decompress.
Review your medications. Talk to your doctor about whether any of your medications might be causing the bitter taste. There may be alternatives.
Try over-the-counter antacids or H2 blockers. For occasional bitter taste from reflux, these can provide relief. If you need them regularly (more than twice a week for more than two weeks), see a doctor instead of continuing to self-treat.
Chew sugar-free gum. This stimulates saliva production, which can help wash away bitter tastes and neutralize acid. Choose mint or citrus flavors.
Rinse with baking soda. Mix half a teaspoon of baking soda in a cup of water and swish it around your mouth. Baking soda is alkaline and can neutralize acids causing bitter taste. Don’t swallow it.
When You Should Definitely See a Doctor
Most bitter taste issues can be managed with lifestyle changes, but certain symptoms mean you need professional evaluation:
If the bitter taste persists for more than two weeks despite home remedies, see a doctor. If you’re also experiencing difficulty swallowing, unintentional weight loss, persistent vomiting, blood in vomit or stool, severe abdominal pain, or yellowing of skin or eyes (jaundice), get evaluated promptly.
Also, if you’re taking over-the-counter antacids regularly for more than two weeks, you need proper diagnosis. Chronic use of these medications without medical supervision can mask serious conditions and cause other health problems.
A gastroenterologist can perform tests to determine exactly what’s causing your bitter taste—whether it’s reflux, bile reflux, gastroparesis, SIBO, or something else—and develop an effective treatment plan.
The Bottom Line
That persistent bitter taste in your mouth is annoying, but it’s usually your digestive system sending you a message. Most commonly, it’s acid reflux—your stomach acid ending up where it shouldn’t be. But it could also be bile reflux, slow stomach emptying, bacterial overgrowth, liver or gallbladder issues, medication side effects, or even just dehydration and stress.
The good news is that most causes are treatable. Simple lifestyle changes—how and when you eat, staying hydrated, managing stress, elevating your head while sleeping—can make a huge difference. For more complex issues, proper medical treatment can resolve the problem.
Don’t just live with that bitter taste, popping mints and feeling self-conscious. It’s your body trying to tell you something. Listen to it, make appropriate changes, and if it persists, get it checked out. Your taste buds (and probably your social life) will thank you.
Get Expert Help for Persistent Bitter Taste
If you’re experiencing persistent bitter taste or other concerning digestive symptoms, Dr. Preetha Thomas, specialist gastroenterologist in Pretoria, provides comprehensive evaluation to identify the underlying cause and develop effective treatment strategies.
Contact us today to schedule your consultation.