You’ve made it through the day. Dinner is done, you’re finally relaxing on the couch, and then it starts — that uncomfortable bloating, the burning feeling creeping up your chest, the gurgling stomach that keeps you awake long after everyone else has fallen asleep. Sound familiar?
If your digestive symptoms seem to reliably worsen after sunset, you’re not imagining it. Nighttime digestive trouble is one of the most common complaints gastroenterologists hear — and it’s not a coincidence that your gut seems to stage its most dramatic protests after dark. There are real, specific reasons why digestion struggles at night, and understanding them is the first step toward actually sleeping through the night again.
Your Body’s Internal Clock Is Controlling Your Gut
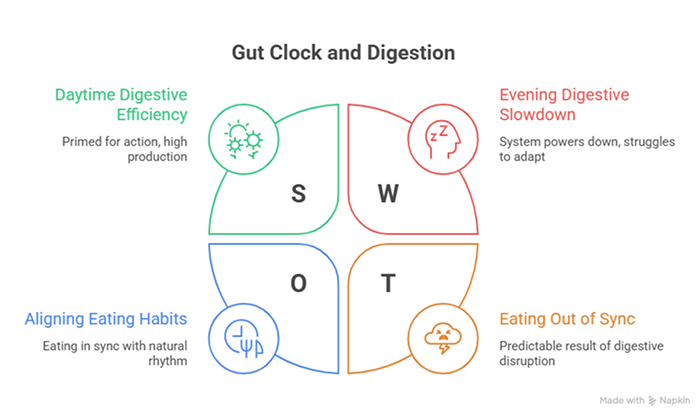
Most people know that the body has a circadian rhythm — the internal 24-hour clock that regulates sleep and waking. What fewer people realise is that your digestive system has its own built-in clock, and it is designed to wind down in the evening.
During the day, your gut is primed for action. Digestive enzymes are produced in higher quantities, gut motility (the muscular contractions that move food through your intestines) is faster, and your liver and gallbladder are more actively secreting bile to help break down fats. As evening approaches, all of this starts to slow. Your gut is essentially preparing for the overnight fast.
When you eat a large meal at 8pm or later, you are asking a system that has already started to power down to suddenly kick into high gear. It struggles. Food sits longer in the stomach. Gas production increases. Acid is more likely to reflux upward. The symptoms you experience are not random — they are the predictable result of eating out of sync with your body’s natural digestive rhythm.
Lying Down Changes Everything
Gravity is one of your digestive system’s best friends, and at night, you take it away.
When you are upright — standing or sitting — gravity helps keep stomach contents where they belong: down in the stomach. The moment you lie down, that advantage disappears. Stomach acid, partially digested food, and bile can now flow far more easily into the oesophagus, causing the burning discomfort known as acid reflux or heartburn.
This is why acid reflux worsens at night for so many people. It is also why going to bed too soon after eating is one of the most reliably problematic habits for anyone with a sensitive digestive system. Most gastroenterologists recommend waiting at least two to three hours after your last meal before lying down — not because it sounds like good advice, but because the physics of your body demand it.
For people who already have a hiatal hernia — a condition where part of the stomach pushes up through the diaphragm — lying down is even more problematic. The anatomy makes acid reflux almost inevitable in certain positions, and symptoms are frequently worst during the night and early morning hours.
Late-Night Eating and the Bloating Problem
There is a reason you feel more bloated at night than you do in the morning, even if you have been eating all day. By evening, your gut has been working for hours, and gas has been accumulating throughout the digestive process. Add a late dinner to the mix, and you are layering new fermentation activity on top of an already gassy system.
Certain foods make this dramatically worse. Cruciferous vegetables like broccoli and cauliflower, legumes like beans and lentils, carbonated drinks, onions, garlic, and foods high in FODMAPs are all fermented by gut bacteria, producing gas as a byproduct. This fermentation happens regardless of what time you eat — but when it happens at night, the gas has nowhere productive to go. You are lying still, gut motility has slowed, and the pressure builds.
Persistent bloating is always worth investigating with a doctor, particularly if it is accompanied by changes in bowel habits, unexplained weight loss, or pain. While nighttime bloating is often related to diet and timing, it can also be a sign of something that warrants medical attention.
Stress Accumulates Throughout the Day — And Your Gut Pays at Night
Here is something that surprises many patients: the stress you experienced at 10am can still be affecting your digestion at 10pm.
Your gut and brain are in constant two-way communication through what is known as the gut-brain axis. When you are stressed, your body releases cortisol and adrenaline — hormones designed to prepare you for fight or flight. Digestion is not a priority in fight-or-flight mode, so your body deliberately slows gut motility, reduces blood flow to digestive organs, and alters the way your intestines function.
The problem with modern stress is that it rarely has a defined end point. Work stress, financial worry, relationship tension — these do not switch off at 5pm. Many people carry a full day’s worth of accumulated stress into the evening, and their digestive systems bear the brunt of it right when they are trying to wind down and sleep.
People with irritable bowel syndrome are particularly vulnerable to this pattern. The gut hypersensitivity that defines IBS means that stress-induced changes to gut function are experienced as pain, urgency, or unpredictable bowel changes — often at the worst possible time. Understanding the gut-brain connection is essential for anyone whose digestive symptoms seem tied to their emotional state.
Gastroparesis: When Your Stomach Empties Too Slowly
For some people, nighttime digestive distress is not just about eating habits or stress — it is a sign that the stomach itself is not emptying properly.
Gastroparesis is a condition where the stomach’s muscular contractions are weakened or dysfunctional, causing food to move through too slowly. People with gastroparesis often feel full long after eating, experience nausea, and notice that symptoms like bloating and discomfort are particularly bad in the evening, after food has been sitting in the stomach for hours.
The condition is more common than many people realise, and it is significantly underdiagnosed because its symptoms overlap with other digestive complaints. It is strongly associated with diabetes (high blood sugar damages the vagus nerve that controls stomach emptying), but can also occur following viral illness, after certain surgeries, or without any identifiable cause.
If you consistently feel as though your food is “stuck” after eating, or if you experience nausea and fullness hours after a meal, it is worth discussing with a gastroenterologist. A condition like this will not improve with dietary tweaks alone — it requires proper evaluation and a tailored management plan.
Small Intestinal Bacterial Overgrowth (SIBO)
Another hidden cause of worsening nighttime symptoms is SIBO — small intestinal bacterial overgrowth. Under normal circumstances, the small intestine contains relatively few bacteria. When bacteria migrate from the colon into the small intestine, or when bacteria in the small intestine multiply beyond normal levels, the result is excessive fermentation of food — particularly carbohydrates — producing gas, bloating, and altered bowel habits.
SIBO symptoms tend to build throughout the day as more food is consumed and fermented. By evening, gas production is at its peak, and the resulting bloating and discomfort can be severe. Many people with undiagnosed SIBO describe their stomach as being visibly distended by nighttime, even though they had no symptoms in the morning.
The condition is diagnosed through a breath test and is treatable, but it requires medical investigation to identify. If your bloating is severe, follows a predictable daily pattern of worsening, and is accompanied by diarrhoea or constipation, SIBO should be on the list of conditions to rule out.
The Medication Factor
If you take medications in the evening — as many people do — some of them may be directly contributing to your nighttime digestive symptoms.
Non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen and aspirin are notorious for irritating the stomach lining and can worsen reflux and stomach pain, particularly when taken on an empty stomach or close to bedtime. Certain antidepressants, iron supplements, potassium tablets, and antibiotics can all cause significant gastrointestinal side effects that may be amplified at night when the gut is already slowing down.
If you are currently on a course of antibiotics, it is particularly important to support your gut health actively, as antibiotics disrupt the balance of gut bacteria and can cause or worsen symptoms like bloating, diarrhoea, and abdominal discomfort — often felt most acutely in the evening hours.
Always discuss the timing of your medications with your doctor or pharmacist. In many cases, simply adjusting when you take a medication — rather than stopping it — can make a meaningful difference to your nighttime comfort.
Sleep Apnoea’s Surprising Link to Digestive Symptoms
This one catches people off guard: obstructive sleep apnoea — the condition where breathing repeatedly stops and starts during sleep — is closely linked to acid reflux and nighttime digestive symptoms.
When you stop breathing during sleep, the pressure changes in your chest and abdomen can actively pull stomach acid upward into the oesophagus. Many people with sleep apnoea wake up with heartburn, a sour taste in their mouth, or a sore throat — symptoms they may never connect to a breathing disorder.
The relationship works in both directions. Reflux can also worsen sleep apnoea by causing throat irritation and swelling. If you snore heavily, feel unrefreshed after what should be adequate sleep, or wake frequently with acid reflux symptoms, it is worth investigating both conditions together rather than treating them in isolation.
Liver and Gallbladder Activity at Night
Your liver never truly sleeps — it performs hundreds of metabolic functions throughout the night, including detoxification, protein synthesis, and bile production. However, gallbladder symptoms often surface specifically at night.
The gallbladder stores and concentrates bile between meals. When you eat a fatty or heavy meal in the evening, the gallbladder contracts to release bile. In people with gallstones or a poorly functioning gallbladder, this contraction can trigger significant pain — often a sharp, intense discomfort in the upper right abdomen that radiates to the back or shoulder. These attacks characteristically occur one to two hours after eating and are frequently worse after evening meals.
Fatty liver disease is also relevant here. Fat accumulation in the liver affects its overnight metabolic function and is often associated with other digestive complaints. If you experience regular pain in the upper right abdomen after eating — particularly in the evening — gallbladder or liver issues should be properly evaluated.
Practical Changes That Can Make a Real Difference
Understanding why nighttime digestion struggles is useful, but what actually helps? These are the evidence-based changes most likely to improve your evenings:
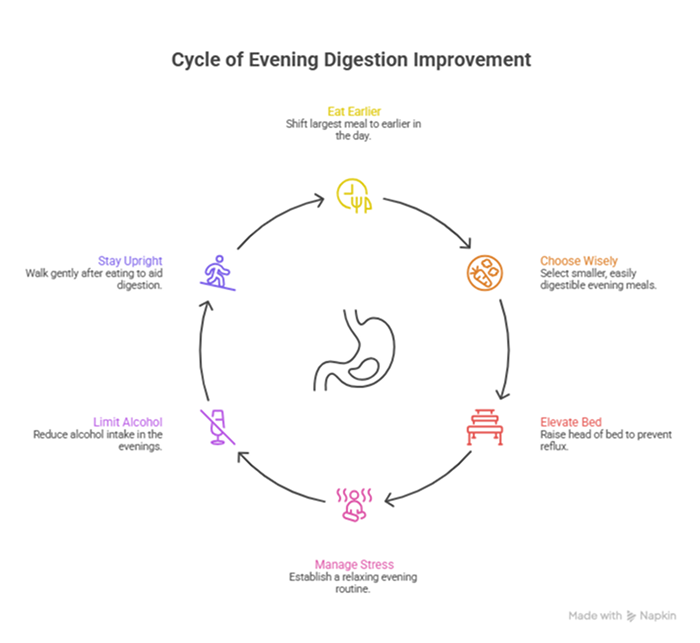
Eat your largest meal earlier in the day. Shift your dietary centre of gravity toward breakfast and lunch. If you are having a substantial evening meal, aim to finish eating at least two to three hours before lying down.
Choose evening meals wisely. Opt for smaller portions and avoid high-fat, high-fibre, or gas-producing foods late in the day. Foods that are easy to digest — lean protein, cooked vegetables, rice, sourdough bread — are your allies in the evening.
Elevate the head of your bed. For those prone to reflux, raising the head of the bed by 15 to 20 centimetres using bed risers (not just extra pillows, which can actually worsen symptoms) uses gravity to keep acid in the stomach during sleep.
Manage your stress before bed. Establish an evening wind-down routine that genuinely signals to your nervous system that the day is over. This might be a short walk, gentle stretching, limiting screen time, or a relaxation practice. The gut-brain connection means that a calmer mind produces calmer digestion.
Limit alcohol in the evenings. Alcohol relaxes the lower oesophageal sphincter — the valve that prevents stomach acid from entering the oesophagus — and significantly worsens reflux. It also disrupts the gut microbiome and interferes with sleep quality, compounding digestive problems.
Stay upright after eating. A gentle walk after dinner is genuinely beneficial — it supports gastric emptying and helps gas move through the intestines more efficiently.
When Nighttime Symptoms Require Medical Investigation
Occasional evening discomfort after a heavy meal is normal. Persistent, regular nighttime digestive symptoms are not something to simply manage around indefinitely.
You should seek medical evaluation if your nighttime symptoms are frequent and disrupting your sleep, if you experience pain that wakes you from sleep, if you notice unexplained weight loss alongside digestive symptoms, if you have difficulty swallowing, if you see blood in your stool or vomit, or if over-the-counter remedies are no longer providing relief.
Early colon cancer can present with subtle bowel changes that are easy to dismiss or attribute to diet. While the vast majority of nighttime digestive complaints have benign explanations, symptoms that persist or worsen deserve proper investigation — not just reassurance.
The Bottom Line
Your digestive system is not designed to work optimally at night. Its internal clock, the effects of lying down, accumulated stress, slower gut motility, and the timing of what you eat all conspire to make evenings a challenging time for digestion. For most people, practical adjustments to meal timing, food choices, stress management, and sleep positioning will produce significant improvement.
But when symptoms are persistent, severe, or accompanied by red flag signs, the message is clear: it is time to stop managing and start investigating. Your gut is trying to tell you something — and a gastroenterologist is trained to listen.
Get Expert Evaluation for Digestive Health
If you are experiencing persistent nighttime digestive symptoms, Dr. Preetha Thomas, specialist gastroenterologist based at Mediclinic Kloof Hospital in Pretoria, provides comprehensive digestive evaluation, advanced diagnostic imaging, and personalised treatment plans to identify the root cause and prevent further progression.
Contact us today to schedule your consultation.