You wake up with a relatively flat stomach. By mid-morning, you notice a slight tightness. By afternoon, your pants feel uncomfortably snug. By evening, you look and feel several months pregnant despite not being pregnant at all. This daily cycle of progressive bloating has become your normal, and you’ve started to wonder if everyone experiences this or if something’s actually wrong.
Occasional bloating after a large meal or during certain times of the menstrual cycle is completely normal. But persistent, daily bloating that significantly impacts your comfort and quality of life? That’s different. That’s your body sending a clear signal that something needs attention.
As a gastroenterologist, I hear variations of this story constantly. Patients describe living with chronic bloating for months or even years, trying every over-the-counter remedy, eliminating random foods, and desperately searching for answers online before finally scheduling an appointment. The question I’m asked most often is simple: “How do I know if my bloating is normal or if I should be worried?”
Let me help you understand when bloating crosses the line from annoying to concerning, what might be causing your persistent symptoms, and when it’s time to seek professional evaluation.
Understanding Normal Versus Problematic Bloating
First, let’s establish what normal bloating looks like. Your digestive system produces gas during the normal process of breaking down food. Some foods naturally create more gas than others—beans, cruciferous vegetables, carbonated drinks, and high-fiber foods all increase gas production. This is actually a sign that your gut bacteria are doing their job.
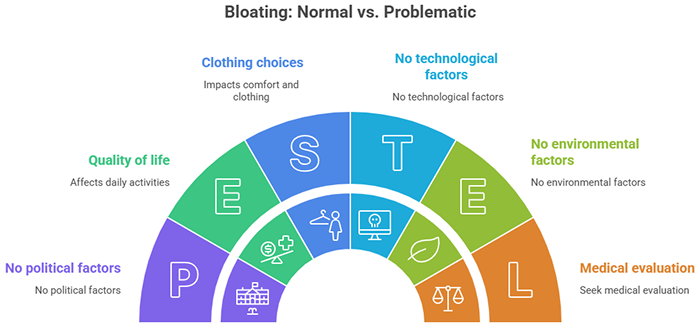
Normal, occasional bloating typically:
- Occurs after specific meals or foods
- Resolves within a few hours
- Doesn’t cause significant pain or discomfort
- Doesn’t happen every single day
- Improves with simple measures like walking or avoiding trigger foods
- Doesn’t progressively worsen over time
Problematic, persistent bloating is different. It’s bloating that:
- Happens daily or most days regardless of what you eat
- Progressively worsens throughout the day
- Causes visible abdominal distension (your stomach actually expands)
- Significantly impacts your comfort and clothing choices
- Doesn’t improve with standard remedies
- Persists for weeks or months
- Accompanies other digestive symptoms
- Affects your quality of life and daily activities
If your bloating fits more into the second category, it’s time to take it seriously and seek medical evaluation.
Common Causes of Persistent Bloating
Understanding potential causes helps you recognize whether your symptoms align with something that requires medical attention.
Irritable Bowel Syndrome (IBS)
IBS is one of the most common causes of chronic bloating I see in practice. This functional disorder affects how your intestines contract and process food. People with IBS experience heightened gut sensitivity, meaning normal amounts of gas and intestinal stretching cause significant discomfort.
IBS-related bloating often:
- Worsens after eating, especially certain trigger foods
- Improves somewhat after bowel movements
- Fluctuates with stress levels
- Accompanies altered bowel habits (diarrhea, constipation, or both)
- Varies in severity from day to day
Many people with IBS also experience frequent stomach noises and gurgling sounds as their intestines react to normal digestive processes with excessive contractions.
Small Intestinal Bacterial Overgrowth (SIBO)
SIBO occurs when bacteria that normally live in your large intestine migrate into your small intestine. These bacteria ferment food prematurely, producing excessive gas in the wrong location.
SIBO causes particularly dramatic bloating, often:
- Starting within 30 minutes to 2 hours after eating
- Creating severe visible distension
- Producing that “looking pregnant” appearance
- Accompanying other symptoms like diarrhea, constipation, or both
- Not improving with typical bloating remedies
The gas production in SIBO can be so significant that people describe feeling like they might burst. This isn’t just discomfort—it’s genuine distress.
Food Intolerances
Lactose intolerance, fructose malabsorption, and gluten sensitivity all commonly cause persistent bloating. When your body cannot properly digest certain foods, bacterial fermentation increases dramatically, producing excessive gas.
Food intolerance bloating typically:
- Correlates with consuming specific foods (dairy, wheat, certain fruits)
- Develops within hours of eating trigger foods
- Accompanies other symptoms like gas, diarrhea, or abdominal cramping
- Improves significantly when avoiding problematic foods
- Returns predictably when trigger foods are reintroduced
Identifying food sensitivities often requires systematic elimination and reintroduction of suspected triggers, ideally under professional guidance.
Constipation
This might seem obvious, but many people don’t realize their bloating stems from chronic constipation. When stool accumulates in your colon, it creates physical pressure and prevents gas from moving through and exiting normally.
Constipation-related bloating:
- Gradually worsens over days without bowel movements
- Improves dramatically after having a bowel movement
- Creates a sensation of fullness and pressure in the lower abdomen
- Often accompanies other constipation symptoms like straining and hard stools
Understanding chronic constipation management becomes crucial since relieving the constipation often resolves the bloating entirely.
Gastroparesis
Gastroparesis involves delayed stomach emptying. Food sits in your stomach much longer than normal, and when it finally moves into the intestines, it can cause significant bloating and distension.
Gastroparesis bloating typically:
- Starts shortly after eating
- Accompanies early fullness (feeling full after just a few bites)
- Often includes nausea
- Worsens with high-fat or high-fiber meals
- Persists for hours after eating
Inflammatory Bowel Disease
Conditions like Crohn’s disease and ulcerative colitis cause intestinal inflammation that affects normal digestive function. Bloating is a common symptom alongside diarrhea, abdominal pain, and sometimes blood in stool.
Celiac Disease
This autoimmune condition triggered by gluten causes intestinal damage that impairs nutrient absorption and normal digestive function. Bloating is one of many potential symptoms.
Ovarian Issues
In women, persistent bloating can sometimes signal ovarian cysts or, rarely, ovarian cancer. This is why persistent bloating in women, especially when accompanied by pelvic pain or changes in urination, warrants thorough evaluation including gynecological assessment.
Red Flag Symptoms That Require Immediate Attention
Certain symptoms accompanying bloating indicate potentially serious conditions requiring prompt medical evaluation:
Blood in your stool (either bright red or black, tarry stools) suggests bleeding somewhere in your digestive tract.
Unintentional weight loss combined with bloating can indicate malabsorption, inflammatory bowel disease, or rarely, cancer.
Severe, persistent abdominal pain that doesn’t improve or progressively worsens needs immediate evaluation.
Vomiting, especially if persistent or containing blood, requires urgent assessment.
Fever accompanying bloating and digestive symptoms might indicate infection or inflammation.
Changes in bowel habits that are dramatic and persist—such as sudden onset of diarrhea or constipation that doesn’t resolve.
Difficulty swallowing or pain when swallowing accompanying bloating suggests esophageal problems.
Family history of colon cancer, inflammatory bowel disease, or celiac disease combined with new, persistent bloating warrants evaluation.
If you experience any of these red flag symptoms, don’t wait—seek medical attention promptly. These symptoms may indicate serious conditions that benefit significantly from early diagnosis and treatment.
When Persistent Bloating Warrants Medical Evaluation
Even without red flag symptoms, certain situations warrant seeing a gastroenterologist:
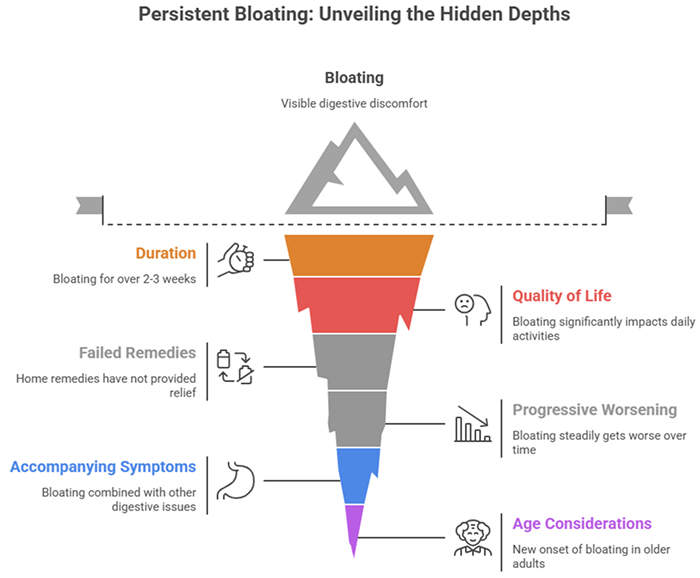
Duration: Bloating persisting daily or most days for more than two to three weeks despite trying common remedies deserves professional evaluation.
Impact on quality of life: If bloating significantly affects your work, social life, ability to exercise, or overall wellbeing, it’s time to seek help. You shouldn’t have to structure your entire life around digestive discomfort.
Failed home remedies: If you’ve tried eliminating common trigger foods, increasing fiber gradually, staying well-hydrated, exercising regularly, and managing stress without improvement, medical evaluation is warranted.
Progressive worsening: Bloating that steadily gets worse over weeks or months rather than staying stable or improving needs investigation.
Accompanying symptoms: Bloating combined with other persistent digestive symptoms like diarrhea, constipation, nausea, or abdominal pain suggests an underlying condition requiring diagnosis.
Age considerations: New onset of persistent bloating in people over 50, especially with no previous digestive issues, warrants more urgent evaluation to rule out serious conditions.
What to Expect During Your Gastroenterology Appointment
Understanding what happens during evaluation helps reduce anxiety about seeking care.
Detailed history: Your gastroenterologist will ask comprehensive questions about your symptoms, dietary habits, bowel patterns, stress levels, medications, and medical history. Be as detailed and honest as possible—there’s no such thing as “too much information” in gastroenterology.
Physical examination: A thorough abdominal exam checks for tenderness, unusual masses, fluid accumulation, or other physical signs of digestive problems.
Initial testing: Blood tests typically check for inflammation, anemia, celiac disease, thyroid function, and other markers of digestive health.
Breath testing: For suspected SIBO or lactose intolerance, breath tests measure hydrogen and methane gases produced by bacterial fermentation.
Imaging: Depending on symptoms, you might need abdominal ultrasound, CT scan, or other imaging to visualize digestive organs and rule out structural problems.
Endoscopy: Upper endoscopy or colonoscopy allows direct visualization of your digestive tract and can identify inflammation, ulcers, polyps, or other abnormalities. These procedures also allow for biopsies to diagnose conditions like celiac disease or inflammatory bowel disease.
Specialized motility testing: For suspected gastroparesis or other movement disorders, specialized tests measure how food moves through your digestive system.
The specific tests ordered depend on your symptoms, examination findings, and suspected underlying causes. Not everyone needs every test—your gastroenterologist will create a diagnostic plan tailored to your situation.
Treatment Options for Persistent Bloating
Treatment depends entirely on identifying the underlying cause. This is why proper diagnosis matters so much—treating bloating without knowing the cause rarely produces lasting improvement.
For IBS: Treatment might include dietary modifications (low-FODMAP diet), stress management, medications to regulate bowel function, and probiotics.
For SIBO: Antibiotics targeting bacterial overgrowth, followed by dietary changes and possibly prokinetic medications to improve intestinal movement.
For food intolerances: Identifying and avoiding trigger foods, digestive enzyme supplements, and gradually expanding food tolerance when possible.
For constipation: Addressing underlying causes, increasing appropriate fiber, ensuring adequate hydration, establishing regular meal and bathroom routines, and sometimes medications.
For inflammatory conditions: Specific medical therapies targeting inflammation, dietary modifications, and in some cases, biological medications.
For gastroparesis: Dietary changes emphasizing easily digestible foods, eating smaller frequent meals, medications to stimulate stomach emptying, and addressing underlying causes like diabetes.
The understanding of gut health connections to stress and overall wellbeing often plays a crucial role in comprehensive treatment approaches.
Self-Care Strategies While Awaiting Evaluation
If you’re dealing with persistent bloating but haven’t yet seen a specialist, certain strategies might provide some relief:
Keep a detailed food and symptom diary. Track everything you eat, when bloating occurs, and severity. Patterns often emerge revealing triggers.
Try an elimination diet carefully. Remove common trigger foods (dairy, gluten, high-FODMAP foods) one at a time for two weeks, then reintroduce while monitoring symptoms.
Eat smaller, more frequent meals. Large meals increase bloating. Five small meals often work better than three large ones.
Slow down and chew thoroughly. Rushed eating means swallowing air and inadequate food breakdown, both worsening bloating.
Stay hydrated. Adequate water intake supports digestion and prevents constipation-related bloating.
Move regularly. Physical activity stimulates intestinal contractions, helping gas move through your system.
Manage stress. Stress directly affects digestive function. Find stress-reduction techniques that work for you.
Avoid carbonated beverages. These introduce gas directly into your digestive system.
Consider probiotics. While research is mixed, some people find certain probiotic strains helpful for bloating.
However, these strategies are temporary measures—they’re not substitutes for proper medical evaluation when bloating persists.
The Bottom Line
Occasional bloating is normal. Persistent, daily bloating that significantly impacts your life is not normal, and you don’t have to just accept it. Your body is telling you something needs attention.
Too many people suffer with chronic bloating for months or years, assuming it’s just “how they are” or feeling embarrassed to seek help for what seems like a minor complaint. But persistent bloating isn’t minor—it’s a symptom that can significantly diminish quality of life and sometimes indicates underlying conditions that benefit greatly from treatment.
If your bloating fits the patterns described in this article—persistent, progressive, impactful—schedule an appointment with a gastroenterologist. Getting an accurate diagnosis is the first step toward effective treatment and finally feeling comfortable in your own body again.
You deserve to live without constant digestive discomfort. Help is available, and most causes of persistent bloating are highly treatable once properly identified.
Expert Evaluation for Persistent Bloating
If you’re experiencing persistent bloating that won’t resolve despite home remedies, Dr. Preetha Thomas, specialist gastroenterologist in Pretoria, provides comprehensive diagnostic evaluation to identify the underlying cause and develop effective, personalized treatment plans.
Contact us today to schedule your consultation.