You’re in your 20s or 30s, supposedly in the prime of your life, yet you’re dealing with persistent heartburn that your parents didn’t experience until their 50s. That burning sensation in your chest after meals, the bitter taste in your mouth when you lie down, the constant need to clear your throat—these aren’t supposed to be problems for young, healthy adults. Yet increasingly, they are.
Acid reflux and GERD (gastroesophageal reflux disease) are skyrocketing among young adults at alarming rates. What was once considered an “old person’s problem” now affects people in their 20s and 30s with increasing frequency and severity. If you’re experiencing acid reflux as a young adult, you’re not alone—and understanding why this is happening can help you take control before it becomes a chronic, life-limiting condition.
The Alarming Statistics
The numbers tell a concerning story. Over the past two decades, acid reflux diagnoses in adults under 40 have increased by more than 50%. Emergency room visits for reflux-related symptoms in young adults have surged. What’s particularly troubling is that younger people are developing more severe forms of GERD earlier, including complications like esophagitis (inflammation of the esophagus) and Barrett’s esophagus (a precancerous condition).
This isn’t just about discomfort. Chronic acid reflux can lead to serious complications: erosion of tooth enamel, chronic cough, asthma-like symptoms, difficulty swallowing, and increased risk of esophageal cancer later in life. When these problems start in your 20s rather than your 50s, you’re facing decades of potential damage unless the issue is addressed.
Why Young Adults Are Suddenly Vulnerable
Acid reflux occurs when stomach acid flows backward into your esophagus. Normally, a muscular valve called the lower esophageal sphincter (LES) keeps stomach contents where they belong. But various factors can weaken this valve or increase pressure in your stomach, causing acid to escape upward.
So why are young adults experiencing this at unprecedented rates? The answer lies in how modern lifestyle factors uniquely affect this generation.
The Obesity Epidemic
Let’s address the elephant in the room: rising obesity rates are the single biggest driver of increased reflux in young adults. Excess weight, particularly abdominal fat, creates physical pressure on your stomach, forcing contents upward. Even being moderately overweight significantly increases reflux risk.
What’s changed is that obesity now affects younger people at higher rates than ever before. Previous generations typically gained weight gradually over decades. Today’s young adults are experiencing significant weight gain earlier in life, often starting in childhood or adolescence, meaning they’re living with reflux risk factors for much longer.
The type of weight gain matters too. Visceral fat (belly fat) is particularly problematic for reflux because it directly compresses your stomach. Many young adults carry excess weight in their midsection, even if they’re not technically obese overall.
The Late-Night Eating Culture
Young adults are night owls. Whether it’s late-night study sessions, working evening shifts, socializing after work, or just binge-watching shows with snacks, eating patterns have shifted dramatically later in the day.
Here’s the problem: your digestive system works best when upright and active. When you eat close to bedtime and then lie down, gravity no longer helps keep stomach contents down. Acid easily flows into your esophagus, especially if your LES is already weakened.
The “don’t eat three hours before bed” rule isn’t arbitrary—it’s based on how long it takes your stomach to empty. But for many young adults, eating dinner at 9 or 10 PM and going to bed at 11 PM or midnight is normal. This pattern practically guarantees reflux, especially if you’re eating heavy, fatty, or spicy foods late at night.
Stress and the Always-On Culture
Young adults today face unique stressors that previous generations didn’t experience at the same intensity. Student debt, competitive job markets, social media pressure, political uncertainty, climate anxiety—the list goes on.
Chronic stress directly impacts your digestive system in several ways. It increases stomach acid production. It can delay stomach emptying, meaning food and acid sit in your stomach longer. It reduces the protective mucus lining of your stomach and esophagus. And importantly, stress can affect the function of the lower esophageal sphincter, making it less effective at keeping acid where it belongs.
The gut-brain connection means that psychological stress manifests as very real, very physical digestive symptoms. For many young adults, acid reflux is partly a stress-related condition.
The Processed Food Diet
Young adults consume more ultra-processed foods than any previous generation. Fast food, delivery apps, meal replacement bars, energy drinks, packaged snacks—these aren’t occasional indulgences but dietary staples for many.
These foods are particularly problematic for acid reflux for several reasons:
High fat content: Fatty foods slow stomach emptying and relax the LES, both of which promote reflux. Fast food meals can contain enough fat to keep your stomach full and valve relaxed for hours.
Excessive sodium: High-sodium foods worsen reflux symptoms, and processed foods are notoriously high in sodium.
Acidic additives and preservatives: Many processed foods contain acidic compounds that directly irritate the esophagus.
Large portion sizes: Restaurant and packaged meals often contain far more food than your stomach comfortably handles, increasing pressure and reflux risk.
The combination of eating large portions of fatty, processed foods late at night while stressed creates the perfect storm for chronic acid reflux.
The Coffee and Energy Drink Epidemic
Caffeine consumption among young adults has exploded, driven by coffee culture and the proliferation of energy drinks. Many young adults consume multiple caffeinated beverages daily—morning coffee, afternoon energy drink, evening soda.
Caffeine is a known trigger for acid reflux. It relaxes the lower esophageal sphincter, allowing acid to flow upward more easily. It also stimulates acid production in the stomach. Energy drinks are particularly problematic because they combine high caffeine with high acidity and sugar—a triple threat for reflux.
The normalization of “needing” multiple caffeinated drinks just to function through the day means young adults are constantly triggering their reflux with substances that directly weaken their esophageal defenses.
Alcohol Consumption Patterns
While overall alcohol consumption might not be higher than previous generations, the pattern of consumption has changed. Binge drinking—consuming large amounts in short periods—is common among young adults, particularly in social settings.
Alcohol triggers reflux through multiple mechanisms. It relaxes the LES. It stimulates acid production. It irritates the esophagus directly. And many alcoholic beverages (beer, wine, cocktails) are acidic themselves, compounding the problem.
The combination of late-night drinking, followed by late-night eating (drunk food is rarely reflux-friendly), followed by sleeping soon after, creates ideal conditions for severe nighttime reflux.
Smoking and Vaping
While traditional smoking has decreased, vaping has exploded among young adults. Both smoking and vaping significantly increase reflux risk. Nicotine relaxes the LES, reduces saliva production (saliva neutralizes acid), and may impair esophageal contractions that normally clear acid.
Many young adults who would never smoke cigarettes regularly use vaping devices, not realizing they’re exposing themselves to the same reflux-promoting effects of nicotine.
The Sedentary Smartphone Lifestyle
Young adults are more sedentary than previous generations, spending hours daily hunched over phones, tablets, and computers. This posture has direct implications for reflux.
Sitting or lying in a slouched position, especially after eating, compresses your abdomen and promotes upward flow of stomach contents. The “tech neck” posture—head forward, shoulders rounded—is particularly bad because it changes the angle of your esophagus in ways that promote reflux.
Additionally, sedentary behavior often correlates with weight gain, creating a vicious cycle where inactivity leads to obesity, which worsens reflux, which reduces activity (because exercise triggers symptoms), which promotes more weight gain.
The Tight Clothing Trend
Fashion matters more than you might think. Skinny jeans, high-waisted pants, tight belts, and compression garments all create external pressure on your abdomen. This pressure forces stomach contents upward, triggering reflux even in people who wouldn’t otherwise experience it.
Young adults, particularly women, are more likely to wear restrictive clothing than older generations who’ve shifted toward comfort. While it’s not the primary cause of reflux, tight clothing absolutely worsens existing symptoms.
Recognizing Acid Reflux in Young Adults
Many young adults don’t recognize their symptoms as acid reflux because they don’t match the “classic” heartburn description. Symptoms can be subtle or atypical:
Classic symptoms:
- Burning sensation in the chest (heartburn)
- Sour or bitter taste in the mouth
- Regurgitation of food or liquid
Atypical symptoms common in young adults:
- Chronic sore throat or hoarseness
- Persistent cough, especially at night
- Feeling like there’s a lump in your throat
- Difficulty swallowing
- Tooth enamel erosion (noticed by dentists)
- Chest pain that mimics heart problems
- Asthma-like symptoms or worsening of existing asthma
- Chronic throat clearing
If you’re experiencing any of these symptoms regularly, especially if they worsen after meals or when lying down, acid reflux is a likely culprit.
What You Can Do About It
The good news is that acid reflux is highly manageable, especially when addressed early. Young adults actually have an advantage—catching and treating reflux in your 20s or 30s prevents the decades of damage that lead to serious complications.
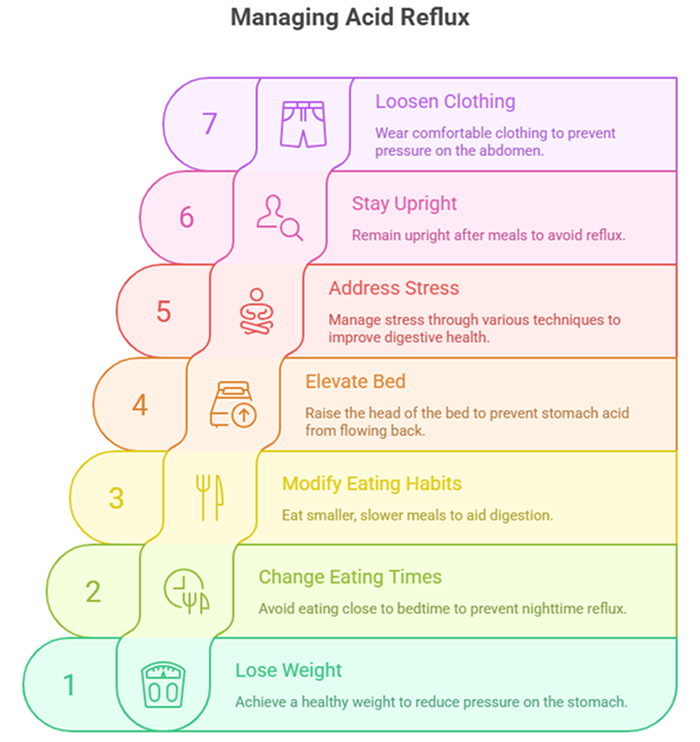
Lifestyle Modifications That Actually Work
Lose weight if overweight: Even a 10-15 pound weight loss can dramatically reduce reflux symptoms. This is the single most effective intervention for many people.
Change when you eat: Stop eating at least three hours before bed. If you work evening shifts or have late schedules, eat your largest meal earlier in the day and keep evening snacks light and bland.
Modify how you eat: Eat smaller, more frequent meals rather than large portions. Chew thoroughly and eat slowly. Don’t lie down or bend over immediately after eating.
Elevate the head of your bed: Raise the head of your entire bed 6-8 inches using bed risers or a wedge pillow. Just stacking pillows doesn’t work because it creates a bend in your torso that actually worsens reflux.
Address stress: This isn’t optional. Stress management—whether through therapy, meditation, exercise, or other methods—is a therapeutic intervention for reflux, not just a nice-to-have. The connection between stress and digestive issues is profound.
Stay upright after meals: Don’t lie down or slump in a chair right after eating. Take a short walk, do dishes, engage in light activity for at least an hour after meals.
Loosen restrictive clothing: Especially around the waist. If your pants leave marks, they’re too tight for digestive health.
Dietary Changes That Make a Difference
Avoid common triggers:
- Coffee and caffeinated beverages (or limit to morning only)
- Alcohol, especially before bed
- Chocolate
- Spicy foods
- Tomato-based foods (sauce, ketchup, salsa)
- Citrus fruits and juices
- Mint (ironically, it relaxes the LES)
- Carbonated beverages
- High-fat foods, especially fried foods
Choose reflux-friendly foods:
- Lean proteins (chicken, fish, turkey)
- Whole grains (oatmeal, brown rice, whole wheat bread)
- Green vegetables (broccoli, green beans, asparagus)
- Root vegetables (potatoes, carrots, beets)
- Bananas and melons
- Ginger (natural anti-inflammatory)
- Healthy fats in moderation (olive oil, avocado)
Stay properly hydrated: Water helps dilute stomach acid and wash acid back down. But avoid drinking large amounts with meals, which can overfill your stomach. Sip water throughout the day instead.
When Medication Is Needed
For mild, occasional reflux, lifestyle changes may be sufficient. But if symptoms persist despite modifications, or if they’re severe, medication may be necessary.
Over-the-counter options:
- Antacids (Tums, Rolaids) for immediate relief
- H2 blockers (Pepcid, Zantac) for moderate symptom control
- Proton pump inhibitors (Prilosec, Nexium) for more severe symptoms
Important considerations:
- Don’t rely on antacids long-term—they mask symptoms without addressing the cause
- PPIs are very effective but should be used under medical guidance, not indefinitely without evaluation
- If you need daily medication for more than two weeks, see a doctor
Many young adults self-treat with over-the-counter medications for months or years without seeking proper evaluation. This is risky because untreated GERD can cause serious damage, and what you think is simple reflux could be something else entirely.
The Importance of Proper Diagnosis
If you’re experiencing frequent reflux symptoms (more than twice a week), severe symptoms, or symptoms that don’t improve with lifestyle changes and over-the-counter medications, you need proper medical evaluation.
Young adults sometimes assume reflux isn’t serious enough to warrant a doctor’s visit. This is a mistake. GERD that starts in your 20s or 30s can cause cumulative damage over decades. Early intervention prevents complications like esophagitis, Barrett’s esophagus, strictures, or esophageal cancer.
Additionally, what you think is reflux could be:
- H. pylori infection requiring antibiotic treatment
- Peptic ulcer disease
- Eosinophilic esophagitis (increasingly common in young adults)
- Cardiac issues (chest pain from reflux can mimic heart problems)
- Other digestive conditions requiring different treatment
Breaking the Cycle
For many young adults, acid reflux becomes a vicious cycle. Symptoms are uncomfortable, so you take antacids. The medication provides temporary relief, so you continue unhealthy habits. Symptoms worsen over time, requiring stronger medications. The underlying causes remain unaddressed.
Breaking this cycle requires commitment to lifestyle changes that might feel inconvenient or socially awkward. Leaving a party early to get home in time to eat three hours before bed. Choosing water instead of that third coffee. Losing weight when diet culture makes healthy approaches difficult. Managing stress when your entire generation feels overwhelmed.
But here’s the reality: the temporary inconvenience of lifestyle changes is far preferable to decades of medication dependence, chronic discomfort, and potential serious complications. You’re young—your body is still resilient and capable of healing. Changes you make now can reverse damage and prevent future problems in ways that become much harder as you age.
The Long-Term Perspective
As a young adult with acid reflux, you have something older patients often don’t: time. Time to reverse damage before it becomes permanent. Time to establish healthy habits that protect you for decades. Time to prevent the complications that develop from years of untreated GERD.
Don’t normalize suffering through daily heartburn because “everyone has it.” The fact that acid reflux is increasingly common in your age group doesn’t make it normal or acceptable. Your body is telling you something needs to change.
The choices you make now—what you eat, how you manage stress, whether you maintain a healthy weight, when you go to sleep—will determine whether acid reflux is a temporary inconvenience of your 20s or a chronic condition that follows you through life.
Get Expert Help for Acid Reflux
If acid reflux is disrupting your daily life, or if lifestyle changes haven’t provided relief, Dr. Preetha Thomas, specialist gastroenterologist in Pretoria, provides comprehensive evaluation to identify the underlying causes of your reflux and develop personalized treatment plans that address your specific triggers and lifestyle.
Contact us today to schedule your consultation.