Constipation has become one of the most common digestive complaints of our time. If you’re struggling with irregular bowel movements, straining, or that uncomfortable bloated feeling, you’re far from alone. In 2026, we’re seeing constipation rates climb across all age groups, affecting people who never had digestive issues before.
What’s changed? Why is something as basic as having regular bowel movements becoming increasingly difficult for so many people? The answer isn’t just about fiber or water intake—it’s about how modern life in 2026 fundamentally conflicts with healthy digestive function.
The Screen Epidemic and Your Gut
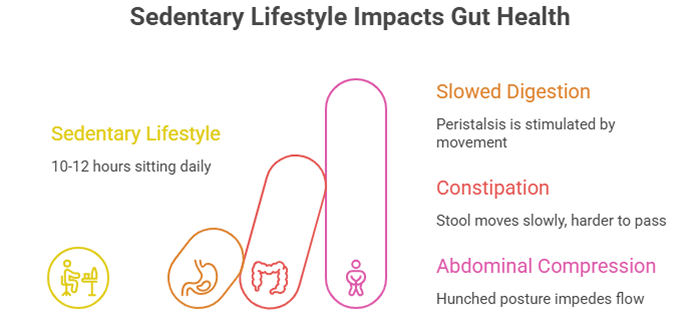
Let’s start with the elephant in the room: we’re more sedentary than ever. The average person in 2026 spends 10-12 hours daily sitting—working at computers, scrolling on phones, streaming entertainment, gaming. Even “active” hobbies have gone digital.
Your digestive system relies on movement. Physical activity stimulates peristalsis—the wave-like muscle contractions that move stool through your colon. When you sit for extended periods, everything slows down. Your colon becomes sluggish, stool moves more slowly, and more water gets absorbed from it, making it harder and more difficult to pass.
Remote work has made this worse. The commute that once provided some movement is gone. The walk to meetings replaced by video calls. Lunch eaten at your desk instead of walking to a restaurant. You might go entire days with minimal movement beyond walking to the bathroom or kitchen.
Even when we’re not sitting, we’re often hunched over phones. This posture compresses your abdomen, physically impeding the natural flow through your digestive tract.
The Ultra-Processed Food Takeover
Food in 2026 is more processed than ever. Meal delivery apps, pre-packaged meals, protein bars replacing actual meals, meal replacement drinks—convenience has completely overtaken nutrition for many people.
Ultra-processed foods are designed for shelf stability, convenience, and palatability—not digestive health. They’re typically low in fiber (the main fuel for healthy bowel movements), high in refined carbohydrates and added sugars, and stripped of the nutrients that support gut motility.
Real fiber comes from whole plant foods—vegetables, fruits, whole grains, legumes. When your diet consists primarily of processed foods, you’re likely getting a fraction of the 25-30 grams of fiber your digestive system needs daily. Without adequate fiber, your stool lacks bulk and moves sluggishly through your colon.
Additionally, many processed foods contain additives and preservatives that can disrupt your gut microbiome—the trillions of bacteria that help regulate digestion and bowel movements.
Dehydration in the Age of Coffee and Energy Drinks
We’re consuming more beverages than ever, but we’re paradoxically more dehydrated. Coffee consumption has skyrocketed, with many people drinking 3-4 cups daily. Energy drinks have become mainstream. Both are diuretics that increase urination and can contribute to dehydration.
Meanwhile, plain water consumption has decreased. People reach for flavored drinks, diet sodas, or caffeinated beverages instead of water.
Your colon needs adequate hydration to keep stool soft and moving. When you’re dehydrated, your colon extracts every bit of water it can from stool, making it dry, hard, and difficult to pass. No amount of fiber helps if you’re not drinking enough water.
The Stress Pandemic
If there’s one defining characteristic of life in 2026, it’s chronic stress. Economic uncertainty, political polarization, climate anxiety, social media pressure, work demands, global instability—the sources of stress are endless and inescapable.
Chronic stress fundamentally disrupts digestive function. When you’re stressed, your body stays in “fight or flight” mode, which suppresses “rest and digest” functions. Your digestive system slows down, blood flow to your intestines decreases, and gut motility is impaired.
The gut-brain connection is powerful. What happens in your mind directly affects what happens in your gut. Anxiety, depression, and chronic stress all manifest as digestive symptoms, with constipation being one of the most common.
Ignoring the Urge: The Busy Life Problem
In our rushed, overscheduled lives, many people regularly ignore the urge to have a bowel movement. You’re in a meeting, on a commute, in an uncomfortable bathroom situation, or just “too busy” to take the time.
This is more damaging than you might think. When you repeatedly ignore your body’s signals, you train your rectum to become less sensitive to the presence of stool. The urge becomes weaker over time. Stool sits in your colon longer, more water is absorbed, and it becomes progressively harder to pass.
Your body has natural rhythms for bowel movements, often triggered by the gastrocolic reflex after eating (especially breakfast). But if you’re rushing through breakfast or skipping it entirely, then rushing out the door with no time for a bathroom visit, you’re working against your body’s natural patterns.
The Medication Factor
More people are taking medications than ever before, and many common medications cause constipation as a side effect:
- Pain medications (especially opioids for chronic pain)
- Antidepressants and anxiety medications
- Blood pressure medications (calcium channel blockers)
- Antihistamines for allergies
- Antacids containing calcium or aluminum
- Iron supplements
- Anti-nausea medications
If you started a new medication around the time your constipation began, there’s likely a connection. Don’t stop medications without consulting your doctor, but do mention the constipation—there may be alternatives.
Sleep Deprivation and Circadian Disruption
We’re sleeping less and less poorly than previous generations. Late-night screen time, shift work, irregular schedules, and chronic sleep deprivation have become normalized.
Your digestive system has its own circadian rhythm. Your gut bacteria follow predictable daily patterns, and digestive processes are optimized during certain times. When you disrupt your sleep-wake cycle—staying up late on screens, sleeping at irregular times, getting insufficient sleep—you also disrupt your gut’s rhythms.
Research shows that poor sleep quality and insufficient sleep are associated with slower gut motility and increased constipation. Your digestive system literally needs consistent, adequate sleep to function properly.
The Microbiome Crisis
Overuse of antibiotics, both in medical treatment and in our food supply, has significantly impacted gut health across populations. While antibiotics are life-saving when necessary, they don’t discriminate between harmful and beneficial bacteria—they wipe out both.
Your gut microbiome plays crucial roles in digestion and bowel regularity. Certain bacterial species produce compounds that stimulate gut motility. Others help break down fiber and produce short-chain fatty acids that feed colon cells and promote healthy bowel movements.
When your microbiome is depleted or imbalanced—from antibiotics, poor diet, stress, or other factors—digestive function suffers. Constipation is often one of the first signs of microbiome disruption.
What You Can Actually Do About It
Understanding the causes is the first step. Here’s what actually helps:
Move regularly: Set timers to stand and move every hour. Take walking breaks. Exercise doesn’t need to be intense—even 20-30 minutes of daily walking significantly improves gut motility.
Prioritize whole foods: Build meals around vegetables, fruits, whole grains, and legumes. These provide the fiber your digestive system needs. Gradually increase fiber intake to avoid bloating.
Drink plain water: Aim for 8 glasses daily, more if you exercise or drink caffeine. Your urine should be pale yellow.
Manage stress: This isn’t optional for digestive health. Find stress-reduction practices that work for you—meditation, exercise, therapy, hobbies, time in nature.
Honor the urge: When you feel the need to go, go. Don’t delay. Try to establish a regular bathroom routine, ideally after breakfast when your colon is most active.
Improve sleep: Prioritize 7-9 hours nightly. Maintain consistent sleep-wake times. Avoid screens before bed.
Review medications: Talk to your doctor about whether any medications might be contributing to constipation.
Support your microbiome: Eat probiotic-rich foods (yogurt, kefir, sauerkraut) and prebiotic foods (garlic, onions, bananas, asparagus). Consider quality probiotic supplements.
Use the right position: When sitting on the toilet, elevate your feet on a small stool so your knees are higher than your hips. This straightens the anorectal angle, making elimination easier.
When to Seek Professional Help
While lifestyle factors cause most constipation, certain symptoms warrant medical evaluation:
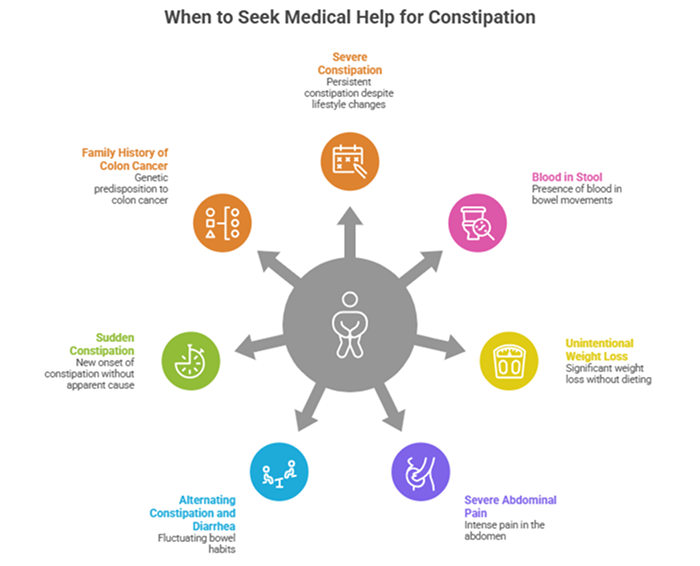
- Severe or worsening constipation despite lifestyle changes
- Blood in stool
- Unintentional weight loss
- Severe abdominal pain
- Constipation that alternates with diarrhea
- New constipation that started suddenly
- Family history of colon cancer
These could indicate conditions requiring specific treatment: hypothyroidism, diabetes, neurological conditions, structural problems, or in rare cases, cancer.
The Bottom Line
Constipation is increasingly common in 2026 not because our bodies have changed, but because our lifestyles have become fundamentally incompatible with healthy digestive function. We sit too much, move too little, eat processed foods, stay chronically stressed, sleep poorly, and ignore our body’s signals.
Your digestive system evolved for a very different lifestyle—one with regular movement, whole foods, natural stress patterns, and adequate sleep. Modern life violates nearly every condition your gut needs to function optimally.
The good news? Unlike many health conditions, constipation is largely within your control. The changes that help—more movement, better food, stress management, adequate sleep—improve not just your digestive health but your overall wellbeing.
If lifestyle changes aren’t resolving your constipation, or if you’re experiencing concerning symptoms, Dr. Preetha Thomas, specialist gastroenterologist in Pretoria, provides comprehensive evaluation to identify underlying causes and develop effective treatment strategies.
Contact us today to schedule your consultation.